Pain has been a gnawing, debilitating and constant companion for Lexi Chambers for the best part of 20 years.
The former Royal Signals soldier, marathon runner and award-winning fitness instructor, has endured eight surgical operations over eight years, starting with the removal of a toe and culminating several years ago with the elective amputation of her left leg.
Along the way, her diary has been crammed with medical appointments, procedures, reviews and an ever-increasing cocktail of painkillers, antibiotics and opiates to quell the excruciating pain that was initially caused by hammer toes and which eventually led to Complex Regional Pain Syndrome (CRPS).
But now, thanks to the pioneering surgery of Lieutenant Colonel Tania Cubison of the Royal Army Medical Corps, the pain is in retreat.
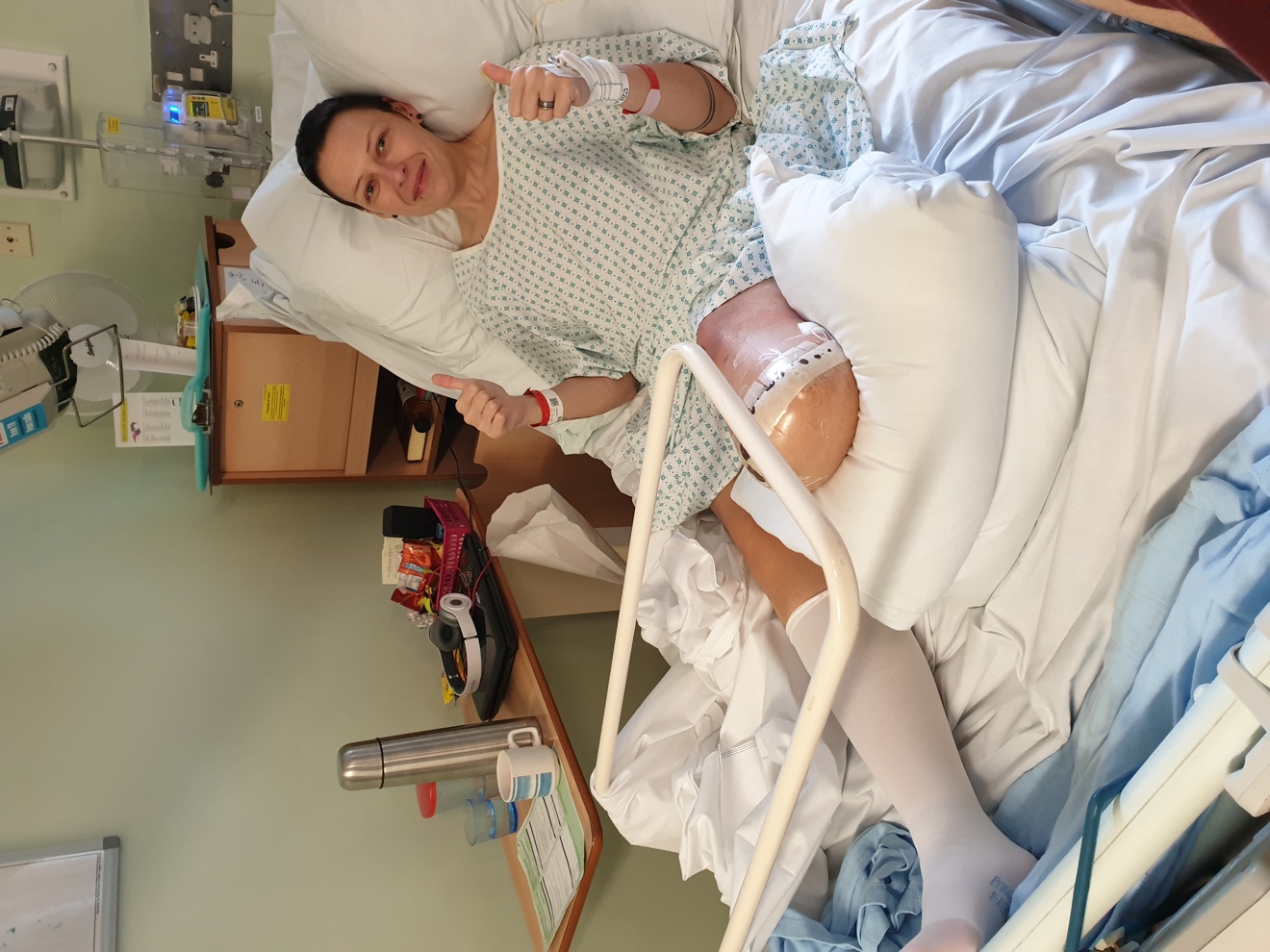
“Tania has literally changed my life,” says 42-yearold Lexi. “I now have hope and can start planning things again. I’ve already signed up to do a triathlon and a half marathon using a wheelchair. Before the operation, I could only focus on the daily battle with the pain – my horizons were incredibly narrow. The pain in my stump had been so bad that I needed heat packs on it 24/7, but the pain is subsiding and today I only need them now and again. I have my life back thanks to Tania and Blesma.”
Cutting-edge surgery

Lexi, from Exeter, is one of around 60 people in the UK who have had Targeted Muscle Reinnervation (TMR) surgery, a procedure that attaches nerve endings, known as neuromas, to other nerves to minimise the pain they cause in amputated limbs.
“I’d had so many consultations and no-one could really get to the bottom of the CRPS. You start to doubt yourself and wonder if it is actually all in your head. To have someone say: ‘I believe you’ and that they could do something about it was incredible,” says Lexi.
“When it was at its worst, I was in constant pain and wouldn’t go out for months at a time. I would get
depressed, which is completely unlike me, but the surgery has reduced the pain and given my life more meaning. I now have the chance to wear a prosthesis, even if it is just for an hour a day.”
CRPS, by its nature, is difficult to define. Medical science is still studying what factors are at play in the body and brain that trigger the high levels of pain that can be a feature of amputation.
Lexi was born with hammer toes; a muscle and ligament deformity that causes the toes to contract, but they initially had little impact on her life. She forged a career in fitness; becoming a UK Fitness Instructor of the Year runner-up, entering natural body building competitions, and joining the Royal Signals at the age of 22.
She left the Army as the pain started to impact her life and retrained as a nurse but had to reduce her hours as CRPS took hold.
“I loved being in the Army, but I was noticing the first signs of pain whenever I ran or after playing football,” says Lexi. “I had orthotics put into my shoes and got permission to wear my own trainers, but it was the start of a nightmare for me. When I became an orthopaedic nurse and saw patients with hammer toes I had the surgeon look at mine and he agreed they needed to be operated on.”
That was the first of eight surgeries that graduated from tendon release to toe and joint removal. But any relief proved to be merely temporary.
“They broke bones then reset them, cut and lengthened tendons, and performed joint release surgery to get more movement in them,” Lexi adds.
“My surgeon predicted that I would be able to run after six to 12 weeks but at the end of that time I was still on crutches, and after six months I was still off work and couldn’t walk.
“I slowly went back to work but had to reduce my hours and couldn’t do anything physical, so it was a miserable time. And it affected my relationship; my wife, Shannon, and I would always cycle and run together but now we couldn’t do that, and she had to see me in constant pain but was unable to help.”
Planning what had been impossible
CRPS, which causes severe, debilitating pain ranging from burning to stabbing sensations, is poorly understood but is thought to be the result of the body reacting abnormally to an injury and disrupting its pain pathways. A study suggests one in 3,800 people develop the condition every year.
The main treatments are self-management, pain relief, psychological support and physical rehabilitation.

“I’d pray that I would wake up the next day and that things would be okay, but the pain was unbearable,” adds Lexi. “I never give up easily on anything so it was very frustrating. The pain continued so I had an elective amputation two years ago but then had to cope with Phantom Limb Pain as well as CRPS.
"I wrote a blog – www.wheelybigchallenge.com – and a reader suggested getting in touch with Tania. When I did, Tania explained that the nerves in my leg were causing mischief because they had nothing to do. The operation attaches them to a muscle to stop them misfiring and causing problems. She was very realistic about the outcome and explained I might only get a 20 per cent improvement, but that was massive to me.”
Tania performed the four-hour operation at the Queen Victoria Hospital in East Grinstead in June, and Lexi’s condition has been steadily improving since.
“I spent a month in hospital gradually getting the pain under control and being able to reduce my levels of pain relief. I still have CRPS but the pain caused by the neuromas and subsequent nerve pain is reducing, which lessens the frequency of CRPS pain flare-ups when my pain sporadically escalates to 10 out of 10.
“Before the operation, I thought I would never be able to walk again, but now I’m thinking I could be cast for a new prosthetic. It has given me a huge psychological lift and I’m planning things that I never thought would be possible, such as doing a wheelchair marathon to raise funds for Blesma and travelling to Everest Base Camp.
“Shannon has seen an improvement already. I used to be moody but now I’m cheery again. Blesma and Steve Fraser [Blesma’s Support Officer in the South West] have been fantastic throughout. Steve’s been with me for every appointment; guiding and advising me, and helping me with my mobility issues.
I had the feeling that my life had almost gone but suddenly having the possibility of doing the things I love again is amazing. I can’t thank Tania or Blesma enough."
The Surgeon's Story
Tania, the RAMC and TMR
The three letters TMR could spell a world of difference for amputees enduring the corrosive force of Phantom Limb Pain. The acronym stands for Targeted Muscle Reinnervation, an innovative surgery that is being pioneered in the UK by Lieutenant Colonel Tania Cubison of the Royal Army Medical Corps who combines her operational role, which has included three tours in Afghanistan, with her position as deputy medical director at a busy NHS Hospital Trust.
TMR was devised by an Austrian physician and involves complex microsurgery performed under general anaesthetic. Tania, who has served with the Welsh Guards, the Royal Regiment of Wales and the Black Watch during a 35-year military career, is one of the first surgeons to perfect the technique, performing the operation on both military and non-military patients in the UK.
“The results have been encouraging, and although it is not perfect, TMR has the ability to change people’s lives for the better,” says Tania, who is a burns specialist as well as a leading expert in stump revision and reconstruction.

Tania’s career spans from a military-sponsored medical degree and RAMC service at the Cambridge Military Hospital, Aldershot, through postings to Catterick, Germany and Afghanistan. She then began work with NHS services and is now part of the leadership executive at the Queen Victoria Royal Hospital in East Grinstead, Sussex.
Focusing on trauma injuries, Tania trained in plastic surgery and burns, and became part of key teams treating military personnel at Selly Oak and Headley Court, as well as in Camp Bastion.
“By the time I got to the hospital at Camp Bastion in 2010, it was very well equipped and full of experienced and skilled professional teams which enabled us to manage the most difficult injuries,” says Tania.
“Everyone knew what they were doing. The teamwork was first rate and often there would be a general, plastic and orthopaedic surgeon working together on one patient, which allowed us to save the lives of very severely injured soldiers.
The complexities of injuries continued to rise from huge energy transfer damage from bigger IEDs and the fact that soldiers carried so much kit. The average soldier weighed in at 162kg – that weight detonated IEDs that might not have been intended for Infantry.
“But the transfer of knowledge and professionalism at Bastion was so good that our automatic thought process came to be: ‘Let’s go in there, do our job and get this soldier back to Headley Court. He’ll be alright.’”
GIVING NEUROMAS SOMETHING TO DO
Phantom Limb Pain (PLP) has been a huge concern for countless amputees since WWI and while its causes are still being researched, the root of the pain is believed to come from the nerves that are cut during an amputation trying to reconnect with their lost ends.
As they misfire they send conflicting signals to the brain which can be interpreted as a range of pain symptoms. TMR takes those nerve endings, known as neuromas, and splices them into other nerves to give them something to do, thereby reducing the range of pain sensations that afflict amputees.
Some 60 people, including Lexi and a number of other Blesma Members, have had TMR surgery and their outcomes are being monitored as medics build a bank of research to inform future treatments.
“We have to be cautious and we are aware that it is not a quick fix. The nerve gets better straight away when you cut it but then it has to regrow and join into the new muscle, which can give patients a pretty miserable time,” says Tania.
“It can take a long time but we have found that it is effective for most people, although for a few it doesn’t work at all. Up until now, there hasn’t been a treatment for PLP so to have a treatment that actually helps is definitely progress.
“Most patients have a significant reduction on their global pain score. Some patients report feeling 75 per cent better all the time, with huge reductions in their PLP, whilst others have two or three great days followed by a rubbish one, and we don’t yet know why that is. One patient is off pain meds and back at work because of the TMR surgery but gets awful pain three times a day for five minutes that she can almost set the clock to.
“We still need to research and understand more but, generally, we are increasingly able to take patients from levels of unmanageable pain and an unworkable quality of life to manageable pain and a place where they can get on with life - even though they may still have bad days.”
We can help
We are dedicated to assisting serving and ex-Service men and women who have suffered life-changing limb loss or the use of a limb, an eye or sight. We support these men and women in their communities throughout the UK. Click the link below to find out the different kinds of support we offer.
Get Support
Leave a comment
Join fellow Members and supporters to exchange information, advice and tips. Before commenting please read our terms of use for commenting on articles.